3 things to keep in mind when going for comfortable 3D imaging in your OR
医疗 4 分钟阅读
3D imaging is a huge asset to minimally invasive surgery, but it can come with discomfort when used for long periods on end. Here are three things you should keep in mind when you want to integrate 3D imaging in your operating room.
Intro: how does 3D imaging work?
In short, 3D imaging works as follows:
- The human eye can only perceive 2D images.
- In order to create a 3D depth effect, we need to ‘trick’ our eyes with a combination of two 2D images: one for each eye.
- The brain combines these, with as result that we have an impression of seeing an image with depth.
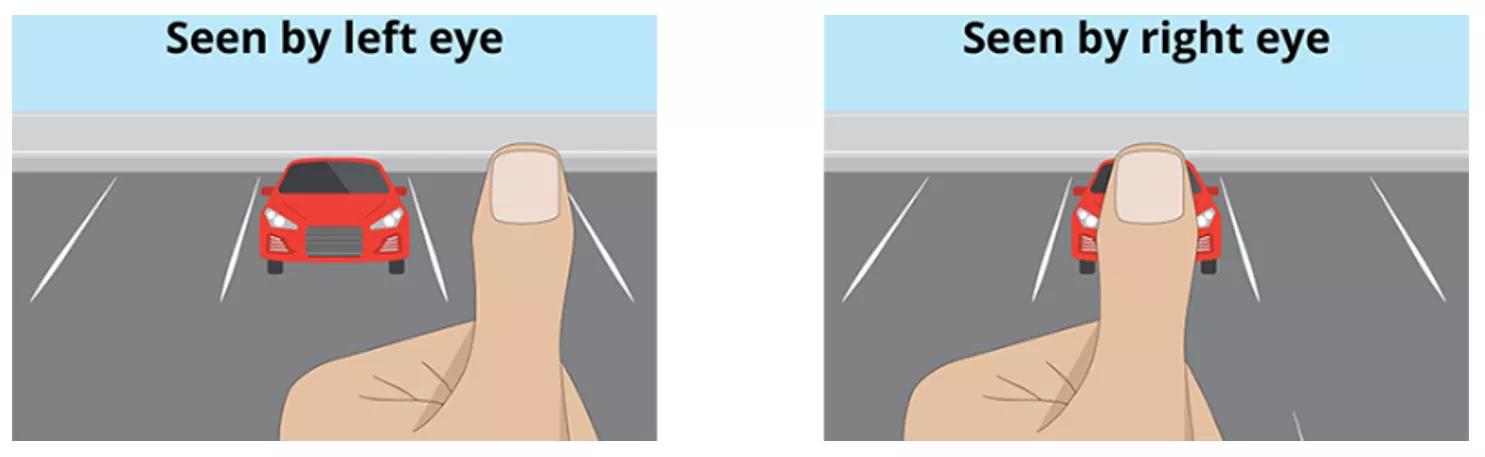
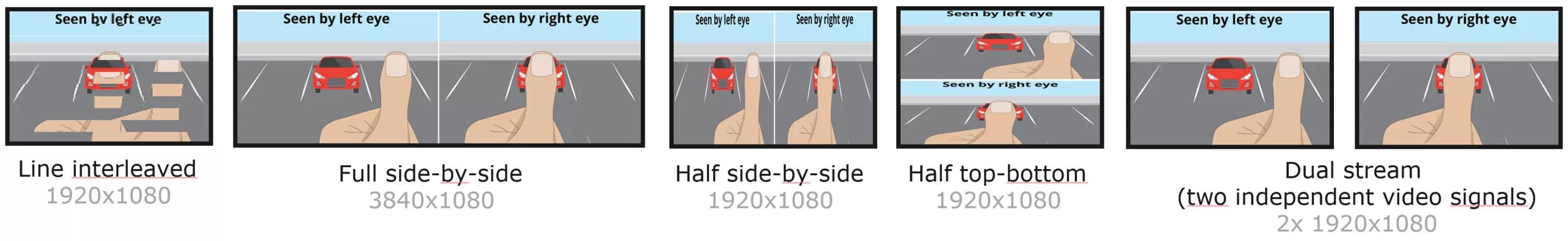
Multiple combinations are possible for two 2D images to result in a 3D image, when viewed through 3D glasses:
3D imaging has found its way into many fields, including surgery – in which the technology probably plays one of its most critical roles. 3D imaging is an important asset to minimally invasive surgery, during which the surgeon uses an endoscope with a camera at its tip to enter the patient, and as such make the physical impact of the surgery on the patient a lot smaller.
It’s important that 3D imaging used in surgery is reliable, just like any other visualization technology. Images must show a near-to-zero latency and no artifacts, and the left and right eye streams must be synchronized perfectly. On top of that, any visual discomfort caused by the 3D viewing must be minimized, so that the OR team can focus on the surgery being done without distraction.
1. Viewing angle
The viewing angle is the angle within which you have optimal view of what is shown on a display. A display has a vertical viewing angle (so from top to bottom) and a horizontal one (from left to right). If the viewing angle is wide, the contents shown on a display will be clearly visible from a bigger area in front of it. When you move out of that area, the screen becomes more difficult to view.
In 3D imaging, a stream for the left eye and a stream for the right eye are displayed simultaneously on the screen, ‘joined’ into one 3D image by your brain, through the glasses that you wear. The horizontal viewing angle of a 3D display is generally similar to that of a 2D display. However, 3D technology can impact the vertical viewing angle of a 3D display.
You might have noticed it that time that you were late to buy your tickets to a 3D movie, and had to sit on the front row of the theater, at the bottom of the screen. Not very comfortable, right?
So when choosing a 3D solution for your OR, remember check the offered viewing angle of the display. It will help you define how and where to place it.

2. Crosstalk
Crosstalk is another specification that you can use to assess how comfortable 3D will be on the eyes during surgery. Crosstalk is a percentage indication of the level up to which the left and right image channel bleed into one another. The effect looks a bit like a double exposure photograph. It is not always very visible but it can make the 3D image harder to process. Ideally, crosstalk remains below 7% to keep visual discomfort at a minimum. This makes it possible to use 3D monitors for longer procedures too.

3. Flexibility
There is no standard in 3D technology for surgical purposes: various 3D types are used, as well as different types of cabling and image resolution. Also, not every surgery requires 3D imaging. So it’s a pity if you cannot maximize the use of your 3D display by switching it to 2D when that’s the better option.
Also, 3D endoscopes are not always part of the digital OR: sometimes, they’re only connected via a cable, so it’s not possible to stream their images outside the OR, or to translate them into 2D on other 2D displays in the OR. Still, these functionalities can greatly improve the flow of a 3D endoscopic surgery. A flexible OR-over-IP system that supports 3D imaging can process various 3D standards, multiple interfaces, and translate a source video automatically into 2D and 3D, depending on each individual display’s possibilities.
By using a 3D display with a wide viewing angle and minimal crosstalk, you increase viewing comfort, especially during long procedures. And with a flexible OR-over-IP system as backbone of your surgery, you can maximize the use of your entire infrastructure, from the camera at the tip of your endoscope to the images your brain processes while operating, be they in 2D or in 3D.

