Why so many tests?
The same goes for our bodies and how they evolve: everyone’s different. That’s a good thing, because the world would otherwise be a dull place. But a side-effect is that the discovery of something suspicious could mean a lot of things. So it’s often the start of a rollercoaster of tests and visits to medical specialists with complex titles.
If you or someone you know is in such a position now, we hope we can shed some light on the road ahead. We’ve summarized it all in an infographic, which you can download at the end of this article. And don’t forget: most breast lumps are not cancerous.
Getting the full picture
The first thing doctors do when they want to investigate something in your breast, is simply mapping it out completely. You can compare it a bit to cartographers. If they map out a geographical area, they’ll be able to understand it better and quicker, including when this area evolves later on.
A map of your breast goes a long way to help the doctors understand what’s going on, where it’s going on, and how your breast is composed. It’s the basis for an accurate diagnosis and efficient future follow-up.
 The first thing doctors do when they want to investigate something in your breast, is simply mapping it out completely.
The first thing doctors do when they want to investigate something in your breast, is simply mapping it out completely.
A ‘map’ of your breast comes in the shape of an image. Just like there are different geographical maps (for example showing roads, population density, or height differences), there are different types of medical images that give information about specific aspects of your breast. The three most common ones used for diagnosis are mammogram, ultrasound, and MRI. In most cases, these suffice to reach an accurate diagnosis of what’s going on. In some cases, a biopsy or additional images are used to be absolutely certain.
Mammogram
A mammogram is an x-ray image of the breast. There are screening mammograms, which are used during normal checkups, and diagnostic mammograms, which are used in case something suspicious was found. Though mammograms are a key part of breast cancer diagnosis, they don’t only reveal breast cancer but can show more benign presences too. An example is fibroadenomas, which are lumps of normal breast cells.
A mammogram is usually taken of both breasts – not because there is something suspicious in both, but because it’s easier to analyze if you compare them with each other. There is also a type of mammogram that is being used more and more that takes a 3D image of your breast. This is called breast tomosynthesis. Mammograms and tomosynthesis make use of radiation, but the doses are very low. They are typically compared to the small extra radiation from the sun that occurs being in an airplane flight. Don’t hesitate to ask the person who guides you through the process for more information in case you worry about this.
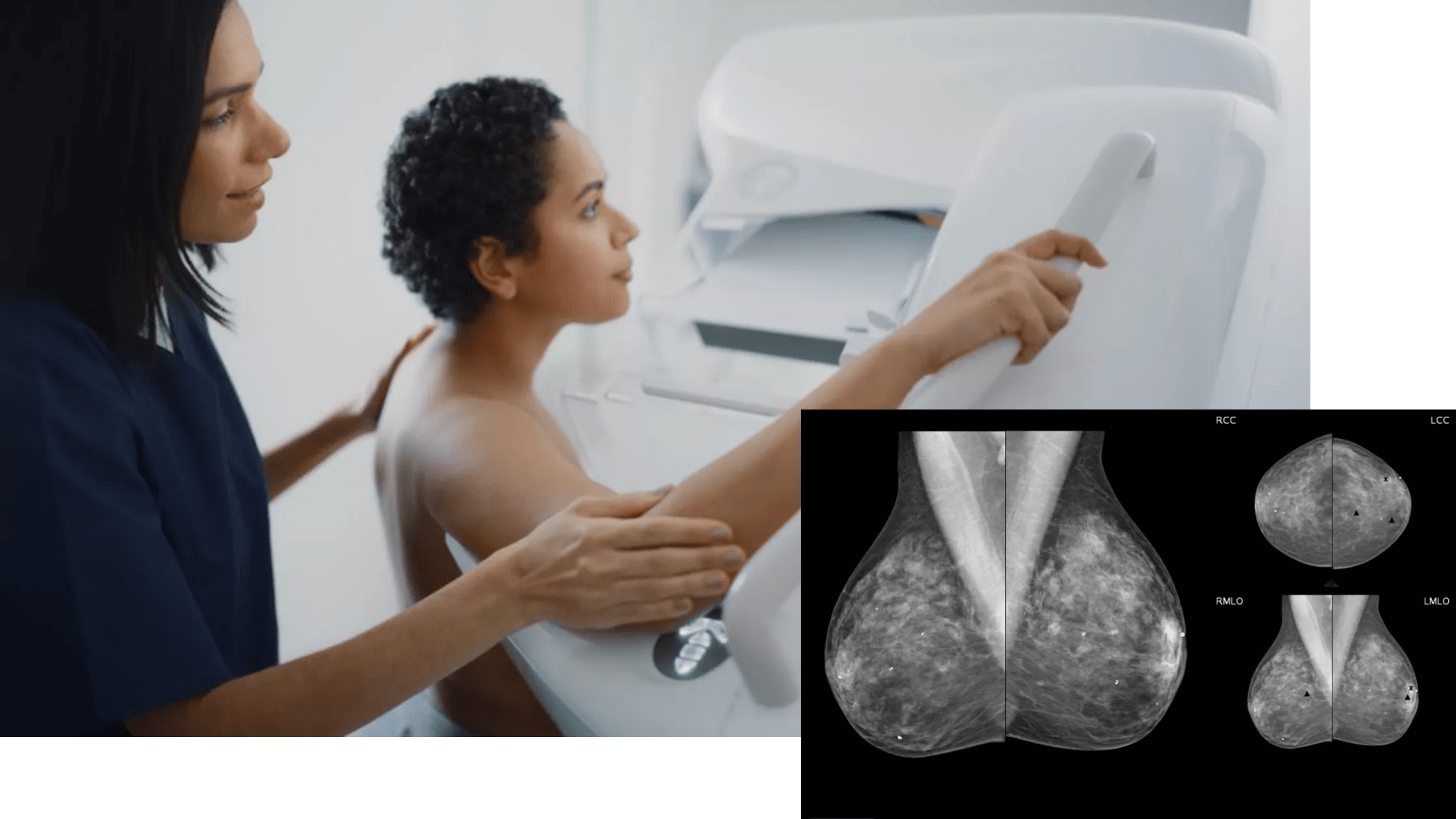
Screening mammograms are used during regular checks, and diagnostic mammograms are used to diagnose when something's been found.
A mammogram shows more detail than an ultrasound, but is more difficult to analyze when the breast is dense. The reason is that solid mass shows white in the image, so lumps that are surrounded by a lot of tissue are more difficult to align. That’s why ultrasound can help in clarifying these dense areas.
Ultrasound
Ultrasound is probably the most common type of image test used worldwide, which you may have had already during a regular visit to a gynecologist or in case you’ve been pregnant. It uses a special gel and sound waves, which make it possible to locate different structures inside your body. You don’t hear the sound because it’s very high-pitched. It reminds a bit of the way in which a bat ‘maps’ its surroundings through sound.
Ultrasound is already more than 50 years old and is an established way to visualize the size, shape and structure of internal organs. It’s also useful to see whether something is a fluid-filled cyst or a solid mass that needs further research. And when a biopsy is needed, ultrasound is often used to guide the needle to the correct spot.
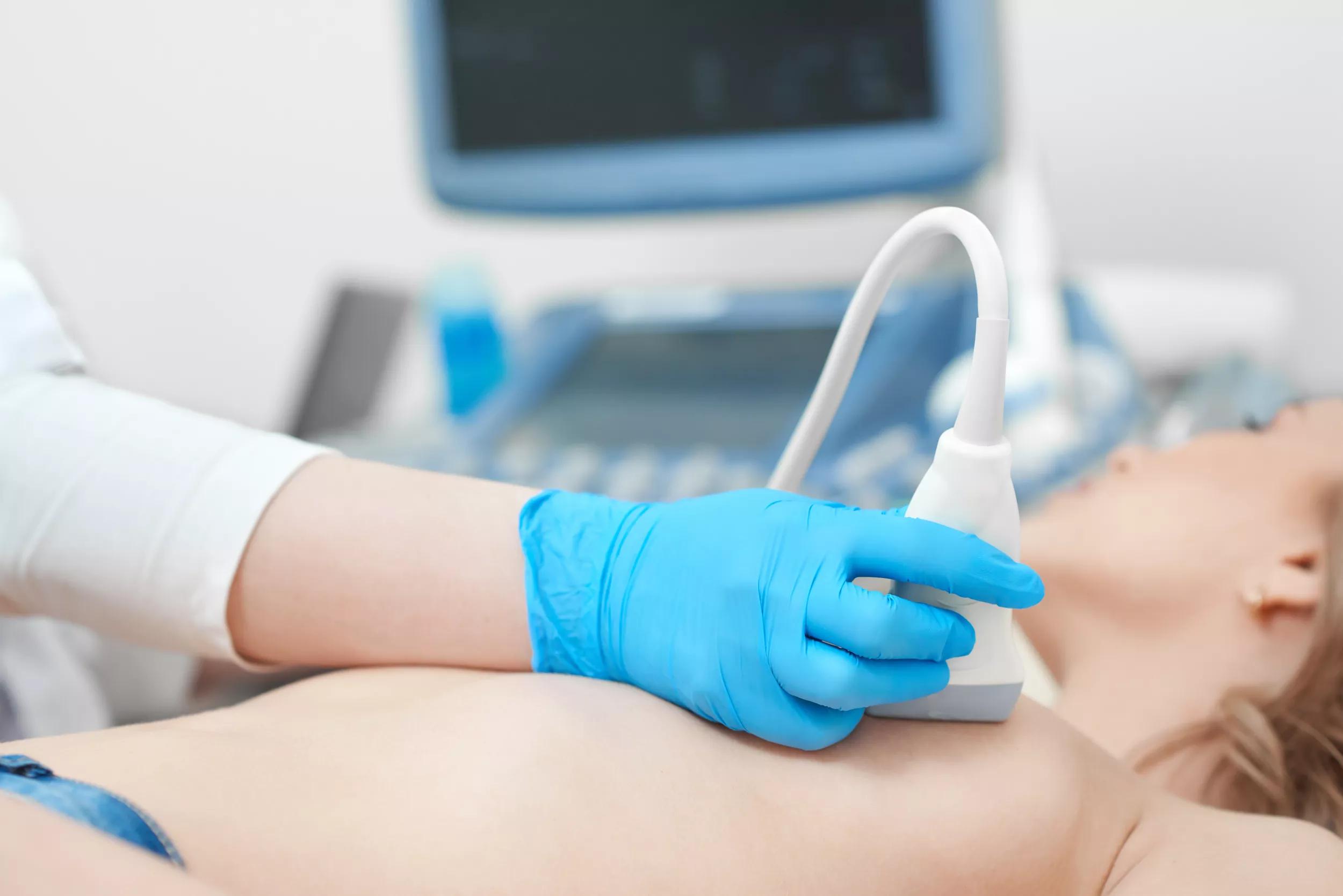
Ultrasound can help the doctor distinguish between fluids and solid tissue.
MRI (magnetic resonance imaging)
Many people will agree that an MRI is the most daunting of the three tests discussed here – the large scanner can make a pretty scary impression. MRI is not always necessary, even when you have already been diagnosed with breast cancer.
An MRI can give a better view of soft tissue than other screening tests, so it’s often used as additional resource. Sometimes, MRI is used as an additional screening test when you have a higher risk factor for breast cancer, just to be sure. Or it can be taken when a breast cancer diagnosis has already been made – for example, to measure the cancer’s exact size.
Remember this: an MRI gives your doctors more information than they already had and can help ruling out incorrect diagnoses. MRI doesn’t use radiation, but radiowaves and strong magnets, which is not harmful for your body. The machine is so big because that simply makes it possible to take images from different angles – it’s as simple as that.
Ask questions!
Do you have any kind of breast image scheduled soon? If you feel nervous about it, that’s perfectly normal – even if it’s a screening checkup. Don’t hesitate to ask your doctor or the person guiding you through the process any question you might have: why you need to do this or that test, or whether it’s possible to go through what will happen together, step by step. There are no stupid questions. You are at the center of this journey.
In our next post, we’ll dive into what happens with your image once it’s taken, and who checks it.




